With one ear on the sound monitor linked to his daughter’s room, Joe Trimarchi sat at his dining room table in the Rosebank section of Staten Island. He was stuffing dozens of envelopes, hoping that one of them would land on the desk of a politician who might care. Mr. Trimarchi, 55, is a cashier in the billing department of Staten Island University Hospital, but what animates him is advocating for his daughter Alexia.
Since she was born 20 years ago with spastic quadriplegic cerebral palsy, a seizure disorder, and hydrocephalus, he has been pestering government agencies and state senators. The Trimarchis have endured two decades of anxiety, hospitalizations and middle-of-the-night scares. But now, the family is facing a full-blown crisis.
When Alexia turns 23, the New York State Department of Health will change her classification from “medically fragile child” to “medically fragile adult.” That distinction, which may seem minor, has enormous consequences. For one thing, Alexia’s caregivers will no longer receive the same hourly rate to which they’ve become accustomed.
The Trimarchis are overwhelmed at the thought of tending to her on their own if that pay cut prompts her nurses to leave. Their other option would be to move Alexia into a nursing home or a group residence, where she would no longer receive one-on-one care.
This is why Mr. Trimarchi spends nearly every night at his dining room table. “We’re fighting for her to have the best life possible,” he said.
Alexia is one of around 1,500 medically fragile children in New York State who depend on Medicaid for private-duty nurses. Children deemed medically fragile require continuous nursing care as well as life-sustaining medications and treatments. In addition, many rely on interventions like feeding tubes, ventilators or supplemental oxygen.
None of them can afford to lose their caregivers. But for the nurses, the situation is untenable: When medically fragile children are deemed adults at age 23, the nurses who care for them lose roughly 30 percent of their pay.
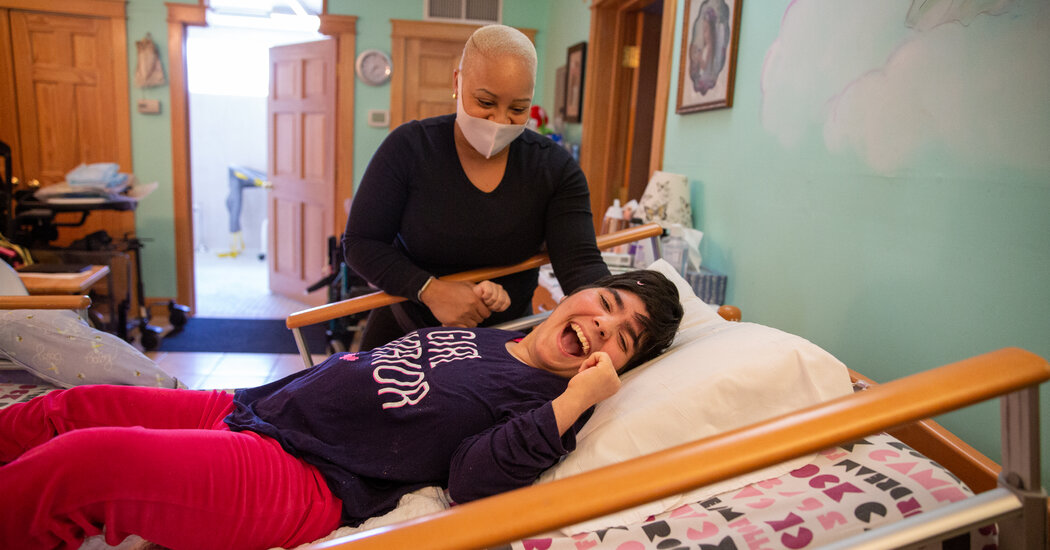
Aziza Hankins, a licensed practical nurse, has been with Alexia since she was a little girl. But in three years, when Alexia is considered an adult, Ms. Hankins’s rate will drop to $23 an hour from $32 an hour, and she fears she’ll have no choice but to leave for a higher-paying job.
“As much as I love Alexia,” Ms. Hankins said, “I’m not going to be able to continue with her. It’s completely unfair, but I have a family to care for, too.”
Medicaid rates for private-duty nursing had been stagnant for more than a decade. Then, in a move many in the industry had spent years agitating for, the Department of Health granted nurses who care for medically fragile children a series of three raises, the second of which went into effect in April. The state also tacked on a 30 percent bump in pay, what it calls an “enhancement.” But all of these financial benefits roll off the table when patients reach adulthood.
Already, private-duty nurses like Ms. Hankins make far less than they would in hospitals, where nurses with comparable skills earn close to a six-figure salary, in addition to health benefits, vacation pay and sick days. As independent contractors, private-duty nurses do not receive benefits. But those who pursue the specialty often do so because they prefer to work with individual patients and want the flexibility of choosing their own assignments.
Still, Ms. Hankins struggles with her decision. All those years spent with Alexia have resulted in a close bond between the two. Alexia is unable to speak, but she and Ms. Hankins have developed their own way of communicating.
“She has a loud personality trapped inside of her body, and she is very specific about things she likes,” Ms. Hankins said. “She has a very hilarious sense of humor. She’s a person like everybody else, it’s just that she happens to be trapped inside of herself.”
Mr. Trimarchi doesn’t want to lose Ms. Hankins. But the Health Department bureaucracy, he says, is so riddled with red tape, illogical hurdles and convoluted regulations that his letters are often ignored for months, if not years. The family already fills in gaps when nurses are forced to miss shifts. He can’t imagine how they could get by if those nurses were to leave for good.
Alexia was born in 2001 at St. Vincent’s Hospital on Staten Island. She was 14 weeks premature and weighed slightly more than two pounds. A series of complications kept her in the neonatal intensive care unit for four months and then in and out of hospitals for the rest of the year.
Speaking on Zoom, Mr. Trimarchi and his wife, Rosina, shared vivid memories of those harrowing months, during which Alexia underwent emergency surgery on her intestines.
“I remember saying to the surgeon, ‘How did it go?’” Ms. Trimarchi recalled. “And he said, ‘It’s in God’s hands.’ And I said to him, ‘Who the hell says that?’ No doctor ever says it’s in God’s hands.”
At that point, the Trimarchis lost hope and called a priest.
But Alexia survived, and the Trimarchis were faced with the daunting task of raising a child who would never walk, talk or feed herself.
They learned how to manage her feeding tube, as well as the frequent infections caused by the shunt inserted in her brain to prevent fluid from accumulating. They also learned how to navigate myriad state regulations; to find and train nurses; and to keep track of an endless stream of medications, supplies and equipment.
Mr. Trimarchi also learned to advocate for Alexia. He successfully fought for a Medicaid waiver to increase her nursing care, first to eight hours a day, then to 12, and finally to 20, where it stands now.
“People at the D.O.H. know me,” Mr. Trimarchi said. “I’ve been sending letters to the Health Department since Alexia was born. They must have 20 years of letters. Oh, they know me.”
But the pandemic presented a new set of problems. Before Covid-19, the Trimarchis had 11 nurses covering 140 hours a week, but the risk of infection reduced their staff to five. Ms. Trimarchi, a speech pathologist with Northwell Home Care, had to cut back her hours to fill the gaps. And their 16-year-old daughter, Adrianna, in between her high school classes and homework, stepped in to assist with physical and occupational therapies, guiding Alexia through biceps curls, leg raises and knee-to-chest exercises.
In December, nine months into the pandemic, Mr. Trimarchi persuaded the Health Department to approve higher-paid registered nurses along with licensed practical nurses to care for Alexia. This allowed him to pull from a larger pool of applicants to fill the empty shifts.
“I was shocked that I got the R.N. rate,” he said. “I think they just figured, ‘He’s a pain in the ass, give him the R.N. rate. Leave me alone.’”
Keeping the medically fragile at home is a relatively new concept. Until the 1980s, most people with severe developmental disabilities were placed in hospitals or large institutions. But hospital care was expensive, and the institutions notoriously neglected their residents.
The most egregious example was Willowbrook, the state-run facility on Staten Island. Housing people with developmental disabilities, Willowbrook State School came under fire for inhumane conditions: Patients were strapped to beds, locked in their wards and left lying in their own excrement. In 1975, a court settlement called for drastic improvements, and 12 years after that, amid public outcry, the state shut down Willowbrook altogether.
By then, New York had begun turning away from institutions in favor of smaller group homes, and more recently it has bolstered in-home care. The financial advantages of keeping those who are medically fragile at home are undeniable. According to Community Resources Staten Island, a nonprofit provider of residential programs, it costs New York State $135,000 to $156,000 per year for a medically fragile child to be in a group home, as opposed to an average of $69,000 for in-home care.
So why the change in nursing-rate reimbursements when a patient reaches his or her 23rd birthday? Given the numbers, why doesn’t the Department of Health encourage in-home care?
Michael DeGrottole, the chief operating officer at Community Resources, offered his opinion. “They just never thought these kids would live into their late 20s, let alone their 30s,” he said. “Now they’re living into their 50s and beyond.”
According to Margaret Mikol, the executive director of SKIP of New York, an advocacy and service agency that helps families navigate the home health care system, the hourly rate for private-duty nurses shouldn’t go down when a patient gets older; it should go up.
“The care doesn’t stop,” she said. “If anything, the older someone gets, the more difficult they are to take care of. Who’s harder to lift? Who’s harder to move?”
The Department of Health has already raised the age cap once. When asked if it had any plans to remove the cap altogether, the department emailed a response to The Times: “Funding was specific to medically fragile children, which previously only covered people to age 21; however, in October 2020, the age was increased to 23.”
Jonah Bruno, director of communications for the Department of Health, added: “We support all efforts to ensure that the most vulnerable New Yorkers receive appropriate care and to ensure their caregivers are compensated fairly.” In addition to raising the age of eligibility to 23, he added that the department “is following through with a $26 million investment this fiscal year on private-duty nursing services that’s projected to nearly double to $51.4 million next fiscal year. No additional changes are being contemplated at this time.”
That disbursement, Ms. Mikol said, was welcome, but she was perplexed that the money did not extend to medically fragile adults.
There was also some hope that the recent federal stimulus would enable the Health Department to lift the age cap. But although the money restored many cuts to programs for those with developmental disabilities, the nurses were left out, Ms. Mikol said.
“We haven’t seen a penny,” she added.
Not all nurses leave when their patients reach the age cap. Patricia Menyuah, an R.N. who trained in her native Nigeria, is one example. Although her hourly rate dropped to $23 an hour from $30, she continues to care for Thomas Ilaridis, a 23-year-old with myotonic dystrophy. The neuromuscular disease has robbed him of the ability to speak, to walk, to feed himself or to breathe on his own.
Thomas’s father, Dimitri, a pharmacist whose wife recently died, worried about how he would manage when Thomas aged out of the system. One nurse left, and another reduced her hours to a single shift a week. But Ms. Menyuah stayed. Her decision came down to a few factors: She lives on Staten Island, an easy two-mile commute to the Ilaridis home; she also likes being responsible for only one patient. Most of all, in the seven years that she’s been caring for Thomas, she has grown attached to him and Dimitri.
To stay on the job — and continue meeting her mortgage payments — she took on a workload of 62 hours a week, sometimes more as needed. That meant forgoing dinner plans, Sunday Mass and time at home with her husband, George Abomeli. It also meant that, during the pandemic, Mr. Abomeli gave up his job as a mechanical engineer, afraid he would catch the virus and infect his wife, who could have passed it on to Thomas.
But Ms. Menyuah sees the positives in what she’s doing. She has two children of her own who are still in Nigeria. “Somebody is taking care of them,” she said. “So why can’t I be happy to take care of somebody like this?”
Well aware that time is running out, Mr. Trimarchi has stepped up his efforts.
“I was always writing letters and stuff,” he said recently. “But the last few years, I started inviting politicians over to the house. Because when you see with your own eyes, it’s better. People don’t understand unless they live it.”
State Senator Diane Savino, a Democrat who represents parts of Brooklyn and Staten Island, was one of those who took Mr. Trimarchi up on his offer. After visiting the Trimarchi home, she weighed the issue, spoke with nursing agencies and came away strongly in favor of eliminating the age cap altogether.
“It’s an illustration of what’s wrong with the way we provide care for medically fragile children,” she said on the phone from her Albany office. “When they hit this magic age and they become medically fragile adults, we jeopardize the very care that they need as they get older. When you cut the Medicaid rate that pays for nurses, it’s a disincentive for them to stay and take care of these young people.”
When asked if she would sponsor a bill to remove the age cap, Ms. Savino said she is working with the Department of Health on the issue. “We’re hoping to do it through the regulatory structure,” she said. “But if we can’t, we’ll introduce legislation to change the funding stream so that it doesn’t revert to a lower funding level at age 23.”
If the age cap remains, the options for Alexia are limited. If the Trimarchis cannot find nurses willing to provide the necessary round-the-clock care, they will most likely need to consider a group home.
The New York State Office for People with Developmental Disabilities serves 120,000 New Yorkers, 38,000 of whom live in group home settings. But according to Mr. DeGrottole, of Community Resources Staten Island, more than a decade of budget cuts has crippled the industry. Group homes are shrinking, merging or on the verge of closing altogether. “People in the industry fear that New York State’s agenda is to reduce the amount of certified beds,” Mr. DeGrottole said.
Besides, he added, most group homes are not equipped to handle the medically fragile. “Residences do exist for the medically frail,” he said, “but they’re very, very few and far between.”
Ms. Mikol agrees that group homes are not feasible for patients like Alexia and Thomas. “We just killed a whole bunch of people who went into nursing homes,” she said, referring to the high toll wrought by the coronavirus. “My God, what would have happened to these kids in a nursing home?”
This is precisely why Mr. Ilaridis chooses to keep Thomas out of a nursing facility. “Let’s face it,” he said, “he will not be getting the same care that he’s getting at home. It’s impossible. The nurses have to have multiple patients, and they’re not going to have the time to attend to him the way we attend to him here.”
The way forward, Mr. DeGrottole said, depends on the state. “They can remove the age cap, or they can start building more group homes to house this population,” he said. “Lifting the age cap would be much less expensive and, frankly, far safer for medically fragile patients. In a group home setting, these types of specialized programs require the appropriate funding. When they don’t get it, we’re in danger of going back to Willowbrook.”
Mr. Trimarchi plans to lobby all 63 New York State senators, pleading for them to lift the age cap, to allow his daughter to stay at home. And so, in the coming months, he’ll be spending his evenings at the dining room table, a stack of papers and envelopes by his side.

Comments are closed.