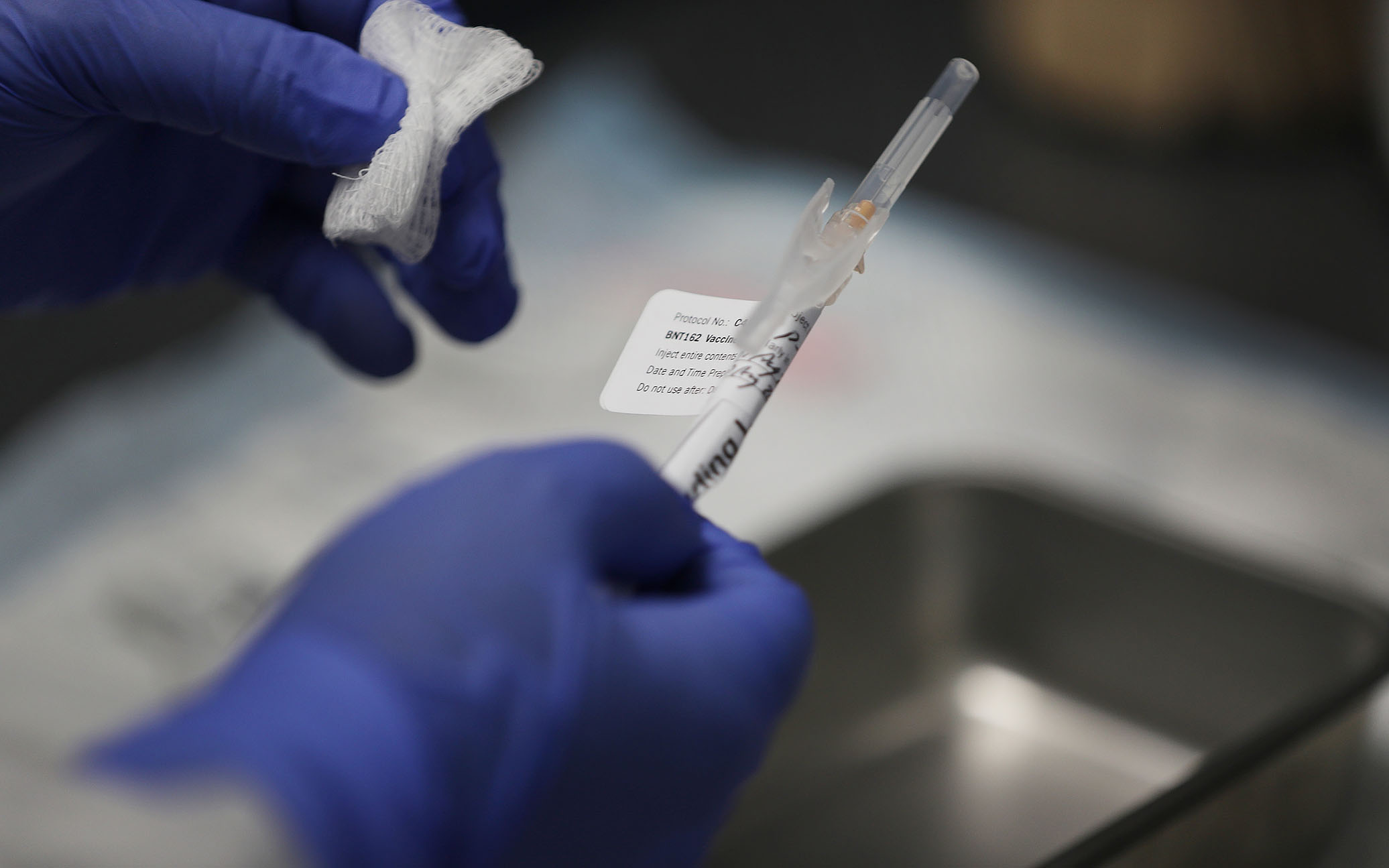
Jose Muniz prepares a COVID-19 vaccination at American research centers in Hollywood, Florida (Joe Raedle / Getty Images / TNS)
People with developmental disabilities are not adequately prioritized in COVID-19 vaccine distribution plans, proponents say, even though they are more likely to die from the virus.
Robert Redfield, director of the Center for Disease Control and Prevention, earlier this month approved a recommendation from the Agency’s Advisory Committee on Immunization Practices on how to distribute initial doses of upcoming vaccines. The shots are expected to be scarce, so access is restricted.
As part of the recommendations, vaccines will initially be distributed to healthcare workers and residents of long-term care facilities. The committee will meet again to determine who should participate in the next phases of the rollout.
Advertisement – Read below
While states are not required to follow the CDC’s Guide to Distribution of COVID-19 Vaccines, most are expected to do so. And that has worried advocates of disability.
Research shows that people with developmental disabilities who become infected with COVID-19 have a two to ten times higher risk of death compared to others. In light of the above, Shannon McCracken, vice president of government relations for the American Network of Community Options and Resources (ANCOR), said that people with developmental disabilities “should be explicitly placed on the top priority.”
“We would certainly expect the message of increased mortality among people with IDD, particularly in groups, to resonate with local, state and state health officials,” said McCracken, whose group represents disability service providers across the country.
According to current CDC recommendations, some people with developmental disabilities might qualify for the first phase of vaccine distribution if they live in a long-term care facility. That probably includes residents of institutions.
“But we are concerned because this is unlikely to include people with disabilities living in group homes, living in support, or receiving services in their own homes,” said Nicole Jorwic, senior director of public policy at The Arc. “That’s a big gap.”
In addition, Jorwic noted that direct support professionals who assist people with disabilities who receive home and community-based services are not a priority. These workers are poorly paid and often work in multiple households, which increases their potential for spreading the virus, she said.
Now advocates are turning to the states that will have the final say in the allocation of vaccines.
“State lawyers need to use the federal recommendations as a starting point and push for better coverage of all people with disabilities and the workforce in any setting in order to get a higher priority for vaccine access,” Jorwic said.
McCracken said ANCOR had written to each of the nation’s governors asking them to classify people with intellectual and developmental disabilities living in a community – including facilities and group homes – as residents of long-term care facility distribution of the COVID-19 vaccine. In addition, the group wants direct support professionals to be considered healthcare workers.
“We would hope that (long-term care facilities) apply to (intermediate care facilities for people with intellectual disabilities) and HCBS programs, as social distancing is virtually impossible when someone is supported in their home,” said McCracken. “Regardless of the recommendations, states and territories still have the power to prioritize critical populations at their own discretion.”