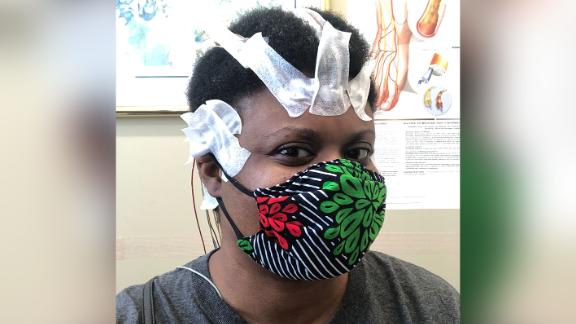
“I was told to go home and rest, that in two weeks everything would be fine. Unfortunately, those two weeks never came for me,” said Chimére Smith, 39, one of many Americans who long against Covid have fought.
According to several studies, long Covid can affect up to a third of Covid 19 patients. Smith is one of them, and people like her can feel the effects of the disease for months, weeks, or, in Smith’s case, more than a year after an acute infection.
A Stanford University study reported that the most common persistent symptoms after Covid-19 were fatigue and difficulty breathing, which affected work ability and other activities. Participants in this study also reported memory problems, loss of taste and smell, and even hair loss.
“I was released”
In late March 2020, Smith, a school teacher from Baltimore, Maryland, went to her family doctor with a sore throat, shortness of breath, dizziness, diarrhea, and difficulty getting up – some of the symptoms that are now from. the US Centers for Disease Control and Prevention are recognized as possible symptoms of Covid-19. In her first month of illness, her symptoms ranged from dizziness to fainting to the feeling that “someone had hit my head on the concrete”.
But, says Smith, “I was fired. I was accused of being fearful and paranoid.”
Meanwhile, her condition continued to worsen as she reported more problems with her eyesight and breathing, as well as neurological symptoms such as memory problems, in the second month of her illness. In the sixth month she could no longer walk.
Smith, who identifies as a black woman, said when she went to doctors – many of whom were white men – they assumed she was a drug addict. One accused her of being “too aggressive” as she tried to dispute her suspicions about what offended her.
“There’s nothing worse than learning that it’s dry eye when you lose vision in your left eye,” said Smith.
She ended up doing more than a dozen Covid-19 tests, all of which came back negative. Antibody tests were also negative. But according to Dr. Igor Koralnik, Senior Physician for Neuroinfectious Diseases and Global Neurology at Northwestern University, it’s not surprising that long-haul flyers test negative for virus particles and antibodies. When the long-distance symptoms set in, patients may stop shedding virus particles and the antibodies in the blood may decrease quickly. (A small study from China found that even patients who were hospitalized sometimes tested negative.)
It’s unclear how many black women are also struggling with long covid, but Smith says she has received an influx of messages from black women like her, who also suffer from long covid-related symptoms, while battling it out To get the care they need. According to the CDC, blacks have a slightly higher risk of contracting Covid-19 compared to whites, and almost three times the risk of being hospitalized for it.
Smith saw her plans to become headmistress dissolve, along with plans to help her mother retire and help her family after her niece was born. “People don’t understand what happens in a black community when a black woman loses her job or is disabled,” she said.
Smith’s activism work with Body Politic, a wellness and legal collective that has long supported Covid patients, has caught the attention of the National Institutes of Health and the CDC. Your contribution with Body Politic made it into the CDC guidelines on caring for Covid patients who “felt like an Olympic torch … Because I’m so proud of the work we were able to do”.
Body Politic has given Smith a community of people with similar experiences who can organize and support one another through the mysterious struggles of Covid. Smith herself has become a spokesperson and advocate for patients like her; She testified before Congress about the impact Covid will have on people and their communities.
And patients are only just getting the recognition they need, she hopes to get better. On July 26th, the Biden administration released guidance stating that long covid could be considered a disability under federal law and thus fall under the Americans with Disabilities Act.
Smith told CNN that her ability to walk is returning, and while she still believes she is disabled, she has made progress on her recovery.
But the secret of Covid remains for a long time.
How Does Respiratory Disease Affect the Brain?
A year and a half after the pandemic began, experts are still puzzling over how a respiratory virus can lead to “brain fog” and memory problems.
“The effects of Covid-19 on the brain are likely to be multifactorial,” says Dr. Dennis Kolson, a neurologist at the University of Pennsylvania who studies the long-term effects of Covid-19 on the brain. He said there was “very limited” evidence that the virus that causes Covid-19 is actually infecting brain tissue. Rather, many of the neurological problems doctors see are likely due to infections throughout the body.
Experts have suggested a number of theories that could explain the long-term neurological effects of Covid-19. The lungs may not get enough oxygen to the brain, or the immune system may be causing so much damage throughout the body that the brain is also affected.
A preprint of an April study found evidence that the virus disrupts cells in tiny blood vessels called capillaries, which would affect blood flow to the brain.
It is also possible that some virus particles themselves are causing damage to the brain, although Kolson says it is unlikely to explain the long-term effects patients see.
What is important, however, is that it is very unlikely that there will be only one correct answer. “Different mechanisms can lead to similar neurological outcomes,” said Kolson.
Doctors examine treatment options
Dr. Michael Saag is an infectious disease doctor in Alabama who treats Covid-19 patients and has lived with Covid himself for a long time. His initial illness included chills, fever, muscle and body aches, loss of smell and taste, “brain fog” and a grueling, night-time cycle of frightening oxygen depletion, which he likened to the movie “Groundhog Day”.
Saag managed to avoid hospitalization. But after his initial symptoms subsided, he found that he wasn’t quite finished with the virus. He was unable to concentrate or think clearly after 2 p.m. every day. Although he has regained some of his hearing, he is now using a hearing aid.
In the early stages of the pandemic, care for its patients living on long Covid was limited. “So from March to April-May we didn’t know anything about long Covid … And when we as a provider went through all of this, we didn’t have much to offer besides holding hands and comfort care.” Saag said.
However, he sees hope on the horizon. “The fact that so many people developed this long-distance syndrome at the same time over the course of a year gives us the chance, the opportunity to study it intensely, and that’s what’s happening right now,” he said.
One of those hopes could be the Penn Neuro Covid-19 Care Clinic, where Kolson is a provider. It is one of several centers formed to care for patients with a range of symptoms after Covid-19, including Northwestern’s Comprehensive COVID-19 Center and the Johns Hopkins Post-Acute COVID-19 Team.
Penn Neuro Clinic uses a “comprehensive approach,” according to Kolson, whereby patients are given a full neurological exam, but are also put in touch with experts from other departments in the Penn system, such as cardiology, and Covid-19 typically affects multiple organ systems . The Northwest Clinic, Koralnik said, does not ask for a doctor’s referral and accepts telemedicine requests from across the country.
More focused studies to understand long Covid are also underway. Koralnik said the Northwestern Clinic is researching the effects of long-term Covid on cognition, sleep, and its ophthalmic effects. The National Institutes of Health have launched their PASC (Post-Acute Sequelae of SARS-CoV-2 infection) initiative. The initiative coordinates and funds a number of studies to understand the effects of long-term Covid and how to treat them. Some websites have already signed up tens of thousands of people to investigate the condition and its causes.
For patients like Smith, recent initiatives are good, but she has stressed the need to involve black women like her. In a University of Washington study that aimed to characterize the persistent symptoms of long-term Covid, only 1.7% of the 177 participants were black. In a study aimed at evaluating risk factors for long covid involving more than 43,000 Columbia University participants, only 22% of participants are black.
“We urgently need the government, policymakers and doctors to get us involved in the research, to keep adequate records of our circumstances and conditions, and to believe us when we tell doctors we suspect we have cases from Covid, “she said.
But there is still more to be done. “I just hope that … [Black women] are not forgotten, “said Smith.” Because I almost was. “
The CNN Wire
™ & © 2021 Cable News Network, Inc., a WarnerMedia company. All rights reserved.